Mycosis Fungoides Symptoms
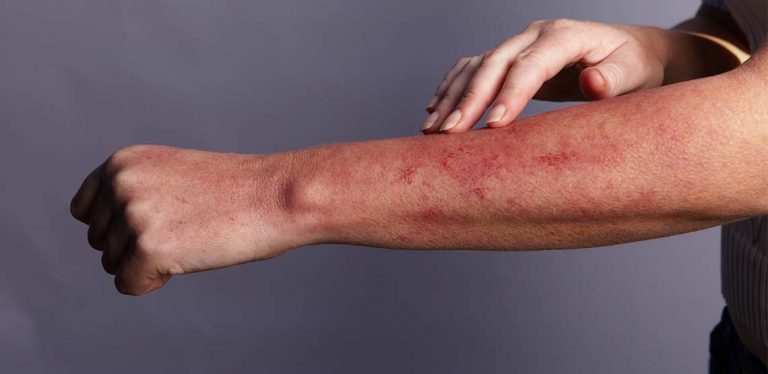
Mycosis fungoides and Sézary syndrome are two types of chronic cutaneous T-cell lymphomas. Cutaneous T-cell lymphoma (CTCL) happens when the body’s T-cells become cancerous. This type of cancer results in what looks like rashes or lesions on the skin. In this article, we will further explore mycosis fungoides symptoms.
Mycosis Fungoides Explained
Mycosis fungoides is one of the most common types of lymphoma. It usually leads to the presence of red rashes on the skin and may progress slowly through different phases. However, not all people go through these phases. Most people initially see patches of skin that are flat, scaly, pinkish, or reddish, but they may not always be itchy.
The last phase of the disease is seen by the presence of tumors. In rare cases, during the tumor phase, the cancerous blood cells can also spread to the organs, such as lymph nodes, liver, lungs and spleen. This increases a person’s risk of developing other lymphomas, such as Sézary syndrome.
Sézary Syndrome Explained
Sézary syndrome is a rarer and more aggressive form of cutaneous T-cell lymphoma. It leads to presence of cancerous cells in the blood, enlarged lymph nodes and extensive rashes, lesions or abnormalities on the skin.
People with this syndrome initially develop reddish and severely itchy rashes called erythroderma, which covers most of their body.
Usually, the Sézary cells are found in the rashes. In mycosis fungoides, the cutaneous T-cell lymphoma affects mostly the skin. In Sézary syndrome, the cancerous Sézary cells spread from the skin to the blood and sometimes lymph nodes, liver, spleen and bone marrow. While mycosis fungoides have several stages and the disease usually progresses slowly, Sézary syndrome spreads fast and is considered an aggressive disease.
Symptoms of Mycosis Fungoides
The main symptoms of mycosis fungoides is the presence of red rashes on the skin. However, because mycosis fungoides progresses in different phases, the signs may look different depending on the stage of the disease.
Stage 1 — Premycotic Phase and Patches
At this stage, you might notice the presence of scaly, red patches that look like rashes in areas of the skin that do not get sun exposure. They may be itchy too. The rash usually will not cause symptoms and may last for months or years. At this stage the person may also experience insomnia.
You may also notice red patches that are mostly found in the upper thighs, lower abdomen, breasts and buttocks. These can sometimes disappear and reappear, but they can stay consistent over time. These are caused by cancerous T-cells, not cancerous skin cells. However, it can be difficult to diagnose mycosis fungoides at this stage.
Stage 2 — Plaques
At this stage, you might notice the presence of bluish, reddish, purplish, or brownish circular or oval plaques that develop in certain body regions (usually the buttocks). Plaques can commonly occur in the same regions as patches, as some plaques can arise from patches, and some develop on their own. These plaques can start as small bumps and later progress into larger plaques and can even coalesce. These can cover up to 10% of the body. For some people these patches may end up developing into tumors, but not in all cases. At this stage you may develop inflammation in your lymph nodes, or a condition called lipomelanotic reticulosis.
Related Search Topics (Ads)
Stage 3 – Tumors
At this stage, clearly noticeable tumors will begin to appear in areas of the skin (usually areas affected by plaques but not always). These tumors are made up of cancerous T-cells and will appear deeper and thicker than plaques. These tumors usually resemble mushrooms, which is why this condition is called mycosis fungoides. These tumors can appear round, bluish, or brownish and be around 1/6 of an inch to 6 inches in diameter. Your skin cells may become thick and lead to necrosis (cell death) of the skin. These tumors are commonly located at the groin area, upper thigh, breasts, armpits and crook of the elbow. The tumors can also develop into open sores that might get infected if not treated properly.
Stage 4 – Disease Spreads to Organs
At the last stage of the disorder, the disease may progress to the rest of the body and cause enlargement of the liver, spleen and lymph nodes. This may lead to feelings of being ill (malaise), weakness, high body temperature, anaemia and weight loss. There may be gastrointestinal issues with possible presence of ulcers in the intestines. A person might also experience coughing and dysphagia (difficulty swallowing). In rare cases, the heart and brain may be affected, and eye pain may occur, leading to blurry vision.
Who is at Risk?
Mycosis fungoides can present in 1 out of 100,000 to 350,000 people with an estimate of 3.6 cases per million people each year in the U.S. Mycosis fungoides makes up approximately 70% of cases of cutaneous T-cell lymphomas globally. Mycosis fungoides is twice as likely to affect males compared to females, and it mostly affects people over the age of 40.
The prevalence of Sézary syndrome is unknown, as it is a rare condition. It is the second most common type of cutaneous T-cell lymphoma and makes up approximately 3% to 5% of cutaneous T-cell lymphoma cases. Sézary syndrome affects mostly adults over 60 and significantly reduces a person’s life expectancy by up to three to four years.
Causes of Mycosis Fungoides and Sézary Syndrome
The cause of both mycosis fungoides and Sézary syndrome are unknown. Some experts believe mycosis fungoides are caused by chromosomal abnormalities. Research suggests it might be associated with variants that help the immune system distinguish the difference between the protein made by viruses and bacteria and protein made by the body.
Also, it has been found that some people with Sézary syndrome also have a human T-cell leukemia virus, which affects their lymphocytes. This can increase one’s risk of developing Sézary syndrome, but this has not yet been extensively researched.
Diagnosis and Treatment of Mycosis Fungoides
Mycosis fungoides is difficult to diagnose. This condition is usually diagnosed through skin examinations and blood tests. It is initially diagnosed by dermatologists or oncologists who specialize in cutaneous lymphomas.
Mycosis fungoides is treated using skin-directed therapies, such as topical steroids, topical nitrogen mustard, retinoids and immune-stimulating creams. Ultraviolet light (medical tanning) and radiation therapy can also be used.
Systemic therapies in the form of pills can also be used for mycosis fungoides, such as bexarotene, methotrexate and vorinostat. Infusion therapies, such as like pralatrextat, romidepsin and immunotherapies, like pembroluzimab, are also used.
Article Resources
- National Cancer Institute [Mycosis Fungoides (Including Sézary Syndrome) Treatment (PDQ®)–Patient Version]
- Cutaneous Lymphoma Foundation (Mycosis Fungoides)
- NORD (Mycosis Fungoides)
- MedlinePlus (Mycosis fungoides)
- Cleveland Clinic (Sézary Syndrome)
- MedlinePlus (Sézary syndrome)
- NORD (Cutaneous T-Cell Lymphomas)